OBESITY AND DIABETES: A CANADIAN EPIDEMIC
Kahnawake is a Mohawk community of 7000 people, located 12 miles north of Montreal, Quebec, on the bank of the St. Lawrence River. Originally settled in 1680, the community traditionally relied on fishing and hunting for food, as well as gathering corn, beans and squash from the area. However, despite the healthy meat and vegetable based diet of the past, today over 800 people (12%), between the age of 45 & 64, live with diabetes (1). Sixty percent of these people are living with major complications, such as blindness and kidney failure; 48% have heart disease as a result of their diabetes. The average age of onset has decreased from 59 in 1985 to 49 in 1995, and more and more children are suffering from the disease. The dramatic rise in obesity and diabetes in this community is attributed the adoption of a Western diet, high in carbohydrates, and a decreased level of physical activity. Obesity related diabetes is an epidemic amongst the aboriginal populations in Canada, and although it presents as extreme within these communities, it is an accelerated model of what is occurring in the general North American population.
People with diabetes cannot regulate their blood sugar levels, and succumb to the devastating complications of the disease, such as heart disease and kidney failure. According to the World Health Organization, over 180 million people worldwide suffer from diabetes and this number is expected to double by 2030 (2). Current unhealthy lifestyle trends in Western society are attributed to the alarming increasing in obesity-related diabetes, and this spread is extending to countries adopting a Western lifestyle. Apart from the imminent health risks and consequences of obesity and diabetes, there are devastating impacts for all Canadians. With increasing childhood onset, as well as the increase in diagnoses amongst the ageing baby-boomers, Canada is at risk of an economic crisis, losing a large portion of its work force to diabetes and related disease. Canadians are also responsible for bearing the cost of this disease, and diabetic patients alone cost the health care system approximately two to three times more than an average patient, creating overwhelming costs. To prevent a Kahnawake-like disaster, Canadians must make major health and lifestyle changes, as well as understand how to rigorously prevent this health epidemic from repeating and spreading. The purpose of this review is to address how the Western lifestyle has blindly promoted obesity, what links exist between obesity and diabetes, and what long-term economic and health implications exist if current lifestyle trends are not addressed.
The Western Lifestyle:
Canada has been steadily growing and evolving into a multicultural mosaic, and provided a home for all different cultures to prosper. As a society, we have prevailed through economic hardship during the first half of the 20th century, and have celebrated our place amongst the leaders of the free, Western world. However, Canada has also evolved like other developed countries into a populace of massive consumers. This culture of consumption, in turn, accounts for factors such as sedentary lifestyle and poor nutrition that has provided a basis for overweight and obese citizens.
Physical activity and proper nutrition form a balance between energy input and output that keeps our bodies healthy and satiated. Physical activity is required for maintaining a healthy lifestyle but it also requires time. Due to our suburban lifestyle, many Canadians commute daily, adding hours to an already long workday. Thus, more and more Canadians are spending their free time sweating in transit than on a treadmill. Vehicle availability to the majority of Canadians also promotes sedentary lifestyle as fewer of us resort to public transport or using manpower, such as walking or cycling to commute to work. Children are also suffering from shortened physical activity due to cuts in physical education programs and the huge popularity of computer games. As a result, more and more children spend time in front of the television, increasing the likelihood of obesity by 10-61% (3). A contributing factor is the loss of green space for parks and recreation, as well as the increasing numbers of children living in complex homes (apartments, condominiums) with little outdoor space. Canadians who participate in sport at a young age have an increased likelihood of maintaining a strong level of physical activity into their adult life (4), and by promoting a healthy lifestyle at an early age, healthy habits are formed. Part of forming healthy habits, however, also includes nutrition and food choice, which is crucial to maintaining a healthy weight.
Energy input is equally as important as energy output. According to Bill Walinsk, Cornell University professor and author of “Mindless Eating”, the average person makes 250 food decisions a day. Whether to eat breakfast, snag another handful of chips or have a midnight snack, we are consciously and sub-consciously balancing energy input versus output. Yet, despite this seemingly trivial task, 47% of Canadians have tipped the scales and constantly eat more than they require (5). Food choices have become increasingly dominated by the “quick-and-easy”. Because of our busy lifestyles, Canadians often reach for pre-made, processed meals or opt for eating out. In addition to being easy, instant meals and fast food restaurants are also cheap alternatives to fresh produce, particularly organic. Fruit based snacks sold at coffee shops or at McDonalds rank amongst the highest priced items, making them even less desirable compared to a muffin or a burger. There is a strong correlation between fast food outlets and lower income suburbs, as well as popular commuting routes, making fast food the cheap and convenient choice for most. As a result of ignoring nutritious choices, our caloric intake has increased 18% since 1991, and our fat intake has increased by 22% (6). Processed foods and refined, baked goods are notorious for only temporarily satiating our hunger, encouraging us to eat more; this is due to their high glycemic index. Glycemic index (GI) is a measure of how fast and how much blood sugar rises after consuming carbohydrates (6). Low GI foods (brown rice, whole grains) cause a slow rise in blood sugar whereas high GI foods (refined flour, white rice, instant oatmeal) stimulate a sudden spike in blood sugar. Constant consumption of high GI foods increases the risk of heart disease and diabetes, whereas low GI foods are shown to help regulate blood glucose in diabetics (6). Living in Canada, we are never short of healthy options, and we must make it a habit to avoid the quick and easy, and think of the long-term.
Obesity:
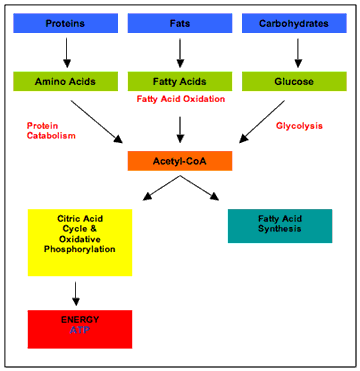
Sedentary lifestyle, poor nutrition and increased food intake has all lead to a serious misbalance in our metabolism. We have tipped the scales so that we are consuming far more than what we need and as a result, too many Canadians are overweight or obese. Obesity is defined as increased body weight due to the excessive accumulation of fat (7). When we consume more than we need, the body acts quickly to store extra calories as fat. When we consume carbohydrates such as bread and rice, they are broken down into single units of glucose through various steps in the digestive pathway (Figure 1). Glucose is then absorbed by intestinal cells and transported to the rest of the body through the blood stream. When a muscle cell, for example, takes up glucose, it is further broken down to acetyl-coenzyme A (Acetyl-CoA) in a cycle called glycolysis and energy is created in a currency form, adenosine tri-phosphate (ATP) that powers cell function. The pathways of fat and protein catabolism also converge at Acetyl-CoA, and this molecule can proceed to the citric acid cycle to create more ATP molecules as energy for the cell. However, when the cell does not need more energy, extra Acetyl-CoA is converted to fatty acids and stored in adipocytes (fat cells) as tri-glycerides. Thus, in order to lose excess fat, one has to create an input energy deficit so the body can only burn what is stored.
Increasing dietary intake of fat saturates adipocytes and creates a condition of high circulating lipids in the blood leading to a high risk of atherosclerosis. Fat resides primarily underneath the skin and in between organs, and distributes differently amongst individuals. However, some cultures are more susceptible to abdominal fat, such as Aboriginals and African descendants, and as a result have an elevated level of inflammation and are at a greater risk for metabolic syndrome, diabetes and heart disease (8). Excess fat is also associated with an increase in cancer, especially breast and colon (8).
The World Health Organization defines obesity using the body mass index (BMI), a measure of a person’s body weight-to-height ratio (2). A healthy BMI is between 20-25, overweight individuals have a BMI between 25-30, and those with a BMI over 30 are diagnosed as clinically obese. Although BMI does not account for muscular tone, it is a fair estimation factor for one’s risk to developing metabolic syndrome, a precursor to heart disease and diabetes, with symptoms such as high blood pressure and elevated blood glucose and fat levels (8). High BMI levels in children are a strong indicator of probable disease in adulthood and decreasing it can diminish many risk factors. Obesity is associated with an array of health risks, however, for the purposes of this review, diabetes will remain the focus.
Diabetes: Type 1 and Type 2
Because of increased dietary intake and adipose tissue in overweight people, the body struggles to maintain proper blood glucose and lipid balance, resulting in chronically high circulating levels of sugar and free fatty acids. Insulin and glucagon are the two hormones responsible for promoting glucose uptake by the tissues, and glucose release into the blood, respectively. Diabetes mellitus occurs because there is a lack of insulin, characterized by high blood glucose levels, and leaving peripheral tissues starved of energy. Type 1 diabetes, also called juvenile diabetes, is classified as the autoimmune rejection of insulin-producing cells called beta-cells, whereas type 2 diabetes is classified as an insensitivity to insulin and impaired insulin secretion. Type 2 diabetes is highly prevalent in overweight and obese individuals because insulin-producing beta-cells cannot produce and secrete enough insulin to lower the excess amount of circulating sugar in the blood. Over time, these beta-cells become exhausted, and insulin processing and secretion becomes permanently impaired. This insulin insensitivity and impaired processing accounts for 90% of all diabetes diagnoses worldwide (2), yet remains to be highly preventable. Type 1 diabetics treat their disease by constantly testing their blood sugars and supplementing with insulin for proper control. Type 2 diabetes can be controlled primarily with exercise and diet control, as well as the use of pharmaceutical agents to increase insulin sensitivity (5). In severe, long-term cases, some patients require injected insulin to decrease blood sugar levels, however the most effective treatment for type 2 diabetes is diet and exercise. Type 2 is a gradual onset and can be left undiagnosed for many years, often left until the late stages. Aboriginal populations are especially susceptible to living with diabetes without a diagnosis due to remote communities and health care services (9). This alludes to the importance of preventative diet choices, and the incorporation of low GI foods to control blood sugar levels. By making lifestyle changes early, type 2 diabetes can be controlled, decreasing the risk of developing major complications.
Economic Burden of Obesity and Diabetes:
With early onset of diabetes in children due to obesity, and an increasing number of diabetes cases in the older, baby-boomer generation, we are facing a health epidemic that could debilitate our economy. Diabetic patients cost our health cares system two to three times more than those without, and this does not account for costs associated with maintaining diabetes, such as medication and supplies (5). Diabetes, and the associated complications, is estimated to cost our health care system $13.2 billion annually, and this number is expected to rise to $19.2 billion by 2020 (5). Other Western countries are not far behind: New Zealand spends 2.5% of all health care expenditures on treating obesity, Australia and France spend 2.0 %, and the United States spends 5.5-6.8% (divided amongst men and women) (3). With massive cuts to our work force, Canada is at risk of a substantial decrease in national productivity due to health, and this forecasts an economic crisis. According to the WHO, China is on course to lose $558 billion in national income due to heart disease, stroke and diabetes. The power economies of the world must prepare for a potential economic crash, and immediate changes must be made to prevent a depleted workforce.
Future Outlook:
Our future is bleak if current trends remain unchanged. The rate of diabetes in Canada is growing faster than our bellies, and statistics like those in Kahnawake will apply to more and more communities across Canada and around the world. Diabetes is a global killer amongst Western societies, and our lifestyles must change in order to prevent a health and economic crisis. However, despite the dreary forecast, even the smallest changes to diet and lifestyle can make a large impact. By incorporating an extra 30 minutes of exercise a day, be it walking to then next bus stop or a brisk walk at lunch, risk factors for diabetes drastically decrease (2,5). Healthy choices can help lower cholesterol, regulate blood sugar and improve energy levels, as well as preventing heart disease. Society is slowly grasping what needs to change, but more pressure must be put on the fast-food industry to stop the spread of processed, convenience foods, and our lifestyles must change to incorporate more physical exercise. An exercise program at the work place is an example of what our employers can do proactively to improve our lifestyles. Many companies are starting to compensate their workers for hours of sitting by supplying compensation for gym memberships, or providing an exercise facility. Providing the opportunity for Canadians to exercise and make healthy choices is the start to a lifestyle change, and society must pressure our governments and employers to support these changes. The food industry is taking major steps to inform us about what we are eating by using nutritional information and healthy choice labels. Even junk food manufacturers are taking steps to make their food less harmful by removing trans-fatty acids (6). All of these changes are collectively improving our health, but the as consumers, we must control our energy balance and take responsibility for this health epidemic. Healthy habits start with the individual, and if we all take steps to think about our health, Canada as a whole will benefit, setting an example for the rest of the world.
References:
1. Macaulay AC, G Paradis, L Potvin, EJ Cross, C Saad-Haddad, A McComber, S Desrosiers, R Kirby, LT Montour, DL Lamping, N Leduc, M Rivard. The Kahawake schools diabetes prevention project: intervention, evaluation, and baseline results of a diabetes primar prevention program with a native community in Canada. Preventative Medicine. 1997 26:779-790
2. WHO: Diabetes. link
3. Birmingham CL, JL Muller, A Palepu, JJ Spinelli AH Anis. The cost of obesity in Canada. CMAJ. 1999 160:483-8
4. “Keeping Kids Active”. link
5. Canadian Diabetes Association. link
6. Peng Y. Canadian trends in obesity and food consumption. Alberta Agriculture, Food and Rural Development. Government of Alberta. February 2004
7. Wikipedia: Obesity. link
8. Goran MI, BA Gower. Relation between visceral fat and disease risk in children and adolescents. Am J Clin Nutr. 1999 70(Supp):149S-56S
9. Young TK, J Reading, B Elias, JD O’Neil. Type 2 diabetes mellitus in Canada’s first nations: status of an epidemic. CMAJ. 2000 163(5):561-5